By Susan Persky
Scientific discovery in the field of genomics is accelerating and will increase understanding of how genetic makeup together with behavioral factors contributes to obesity and its co-morbidities. However, determining how to optimally incorporate this new knowledge into medicine and public health to prevent and treat obesity will be a considerable challenge in coming decades. Currently, we know very little about how patients and health care providers will respond to genomic information and the impact it will have on their decisions and behavior. To ensure effective translation, researchers need to evaluate possible impacts of genomic knowledge ahead of its application. Our research group in the Social and Behavioral Research Branch of the National Human Genome Research Institute uses immersive Virtual Reality (VR) research tools to do exactly that.
In our Immersive Virtual Environment Testing Area, we explore these anticipated situations through VR-enabled research. My collaborators and I attempt to identify optimal ways of integrating genomic information into clinical encounters with patients who are overweight or obese. We aim to discover ways that this information can promote positive social outcomes, for example, reducing stigmatization of patients based on their weight. At the same time, we also investigate if and how genomic information can promote healthy dietary and physical activity behavior.
To explore these issues, we developed a basic VR-based clinical encounter simulation. Using this tool, my collaborator Dr. Collette Eccleston and I investigated how providing information about genetic underpinnings of obesity to medical students effected patient care and treatment. Because the patient in the study was virtual, we could manipulate whether she appeared to be obese or not while holding all other variables constant. The virtual patient told medical students about her symptoms and concerns, and medical students were asked to advise and make decisions about the patient’s care while we tracked their responses and behaviors. This research demonstrated that providing information about the genetic underpinnings of obesity as part of a clinical encounter with an obese patient reduced the extent to which medical students stereotyped and avoided eye contact with that patient. At the same time, however, it also reduced the rates at which they recommended health behavior and weight management consultation as part of her care. The latter outcome raised concerns that dissemination of genomic knowledge could undercut efforts to engage patients in health-promoting behaviors.
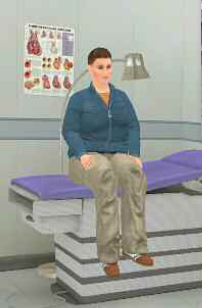
Figure 1: Screen shot from the Immersive
Virtual Environment Testing Area featuring
the clinical encounter simulation.
In current work, my collaborators and I examine the effect of physician-provided genetic information on patients who are overweight. In the virtual clinic, patients encounter a physician who administers weight counseling information while using different communication approaches. In this way, we can investigate whether these communication approaches might mitigate negative social or behavioral consequences or amplify positive consequences of providing patients with genetic obesity risk information.
We initially chose to employ VR methods for this research as opposed to more traditional ones (e.g., hypothetical vignettes, standardized patient or clinician actors) for a few important reasons. In the VR clinic our participants can directly experience and respond to situations that are forecast to occur in the future, but are not yet a reality. At the same time, we can study aspects of the scenario (e.g., the type of genomic information introduced, the communication approach of the clinician) in a manner that is standardized between participants. We also use VR to embed measures of behavior, like a clinician’s level of eye contact with a virtual patient, in the research context.
Moving beyond the clinical context, we have also developed immersive VR environments that serve as stand-alone behavioral measures. We recently created a VR model of a buffet restaurant for an ongoing study in collaboration with Dr. Colleen McBride. The study investigates how the provision of genomic information about a young child’s obesity risk affects mothers’ food choices for that child. In the virtual restaurant mothers fill a plate with various foods. We measure calorie content of the food choices to provide a rigorous behavioral outcome. Although the VR restaurant currently lacks some sensory modalities (e.g., smell), it does offer practical benefits and allows sensitive measurement of mothers’ engagement with the food (e.g., food choice order).

Figure 2: Screen shot from the Immersive
Virtual Environment Testing Area featuring
the VR model of a buffet restaurant.
The application of VR tools for obesity prevention and treatment research is still relatively rare. Our goal in the Immersive Virtual Environment Testing Area is to build a collection of VR research scenarios that will enable us to investigate new questions related to genomic applications for weight management and obesity prevention as they emerge in step with scientific advancement.
Susan Persky, Ph.D. National Human Genome Research Institute National Institutes of Health USA perskys@mail.nih.gov http://www.genome.gov/27533900
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.