By Christopher R. Jones, Ricardo B. Cardoso & Thais Russomano
Metabolic syndrome describes a collection of risk factors that are primarily associated with the development of diabetes and coronary artery disease, but have also been implicated in non-alcoholic fatty liver, stroke and certain cancers. Chronic non-communicable diseases such as these are responsible for 60% of global deaths and cardiovascular diseases are leading the way. The morbidity and mortality attributable to these conditions are enormous and highlight the need for expeditious management and risk factor prevention. Worryingly, the number of people displaying features of the metabolic syndrome is increasing all over the world. Specifically, 25% of the adult population in Europe and the Americas are thought to meet the syndrome’s criteria.
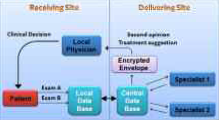
Most patients with metabolic syndrome can be adequately managed within primary care, where the family physician will address each component individually in order to prevent future problems. However, there will be some complicated cases that require specialist input, such as evaluation by a cardiologist or an endocrinologist, in order to prevent or treat complications. A recent overhaul of the Brazilian health system has improved primary care access to a level that would previously have been unimaginable and the consequent progress in public health is encouraging. Nevertheless, problems still remain – Brazil is a country of continental proportions that experiences significant social and health inequalities and access to specialist care is poor outside of big cities. This provides the perfect arena within which eHealth can flourish. The eHealth revolution is upon us. Technology has penetrated every aspect of healthcare at an unprecedented rate, from an organizational and administrative level to the front-line delivery of services. It is simultaneously enhancing the quality of healthcare provided and reducing costs; thus it comes as no surprise that eHealth is working its way up the political agenda, both nationally and internationally.
At Pontifícia Universidade Católica do Rio Grande do Sul (PUCRS) we have organized several successful telemedicine projects over the last five years. The focus has been on specialist second opinion delivery in remote areas of Brazil covering dermatology, cardiology, odontology, ophthalmology and pharmacology. In July 2010, we conducted a multidisciplinary eHealth assistance project in a remote region of the Brazilian Amazon in collaboration with the State University of Amazonas (Figure 1). Through this project we were able to provide rural Brazilians with access to secondary care without them having to leave their communities. There were many patients with features of metabolic syndrome, some of whom were not being managed optimally. Recommendations were made for future management that will hopefully help to prevent the development of serious complications.

Figure 1: A
community in a remote
region of the
Brazilian Amazon
that participated in
the eHealth project.
An underlying theme of our work in Brazil has been to provide people living in remote areas with access to specialist care via telemedicine that they may otherwise not receive (Figure 2). Although Brazil has good access to primary care, the area of medicine that traditionally caters to the components of metabolic syndrome, many countries in the world do not. Rural healthcare in such countries is delivered by non-medically trained community health workers. Our model could be used by community health workers to interact with physicians and optimize management of patients. Furthermore, it provides a reliable source of information for those community health workers wishing to further their knowledge. We believe that our multidisciplinary eHealth model could potentially be adapted and applied in any setting around the world with access to an Internet connection.
One of the key barriers to the adoption of Internet-based telemedicine initiatives in many countries is a lack of bandwidth; some remote areas do not enjoy any Internet coverage. On the other hand, the mobile network is present almost universally. Mobile device technologies (e.g., mobile phone, PDA) for healthcare, or “mHealth,” have been used in many different contexts. Not only are they relatively cheaper, network coverage is also more extensive and reliable than the Internet. Furthermore, more than 75% of the world’s population use a mobile phone. They have been used for ongoing medical education, community and clinical data collection, real-time monitoring of vital signs and second opinion delivery using transmitted images. In more affluent countries iPhones have become commonplace within hospitals.
The potential of eHealth is encouraging and will undoubtedly offer effective solutions for some of the current inefficiencies in healthcare delivery in many regions of the world. It is of the utmost importance, however, that any initiative is carefully considered to ensure that it is culturally and contextually appropriate. Any intervention should be designed based on the specific area within which it will operate. A one-size- fits-all approach will inevitably fail.
Dr. Christopher R. Jones, BMS Eng. Ricardo B. Cardoso Prof. Thais Russomano, M.D., MSc, Ph.D. Pontifical Catholic University of Rio Grande do Sul Brazil christopher.r.jones@doctors.org.uk
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.