➣ By Teresita Marie Sotomayor & Don Parsons
During the Vietnam War over 2,500 Soldiers died due to hemorrhage from extremity wounds. In current conflicts hemorrhage continues to be the leading cause of preventable death in combat, therefore, it is the responsibility of every Soldier to know how to control hemorrhage on the battlef ield. For most extremity wounds the use of a temporary tourniquet has been essential in stopping life-threatening hemorrhage. If the wound is not an extremity wound and a tourniquet is not applicable as in the case of neck, axillary, and groin injuries, the application of a hemostatic agent with pressure is necessary to control the bleeding. The location of the wound is the factor that drives the tools necessary to control the bleeding. The more proximal the extremity wound the more difficult the application of a tourniquet. These types of wounds currently necessitate the use of a hemostatic agent in addition to direct pressure and eventually a pressure bandage to control bleeding. Wounds of the axilla, groin, and neck can be fatal if a means of controlling the hemorrhage is not readily available.
Frequently, medics rely solely on tourniquets to stop bleeding for extremity wounds. However, they need to have the experience of attempting to use a tourniquet that may not work on a very proximal wound. This requires them to reevaluate their intervention and successfully transition to another hemorrhage control measure if their initial attempt is unsuccessful. In addition, hemostatic agents are also taught as a means of transitioning away from a tourniquet in the event of a delayed evacuation and the possibility of extremely prolonged use of a tourniquet. Hemostatic agents are substances that promote homeostatic coagulation when applied to a hemorrhaging injury. Use of such agents has drastically reduced the number of deaths that could be prevented on the battlefield. In the last decade, significant advances have been made on hemostatic agents. Each class of hemostatic agent differs in application and mechanism of action; combat gauze is currently the agent recommended for use by the U.S. Army. There is currently a package of combat gauze in every Soldier’s Individual First Aid Kit (IFAK), and in every combat lifesaver’s and combat medic’s aid bags.
Army Combat Training Schools and medical simulation training centers rely on simulated capabilities to conduct realistic hands-on training and evaluation of hemorrhage control using tourniquets and hemostatic agents.
The U.S. Army Simulation and Training Technology Center (STTC) Human Dimension, Simulation and Training Directorate, Army Research Laboratory (ARL) executed a three-year (FY07- 10), joint Army Technology Objective (ATO) with the U.S. Army Medical Research and Materiel Command (MRMC), entitled Severe Trauma Simulations. The mission of the ATO was to research and develop innovative technologies to realistically simulate the look, feel, and smell of severe trauma to prepare medics, combat lifesavers, and Soldiers to deal with the injuries encountered on the battlefield. The results from this effort produced enhanced tools for realistic medical training enabling the Army to maintain better trained medics and to improve the ability to save lives on the battlefield.
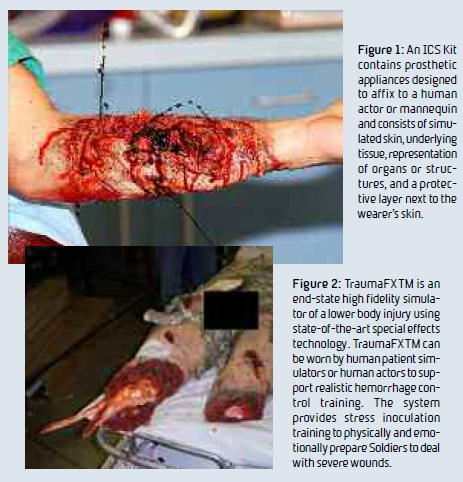
By merging the latest special effects technology with material science research, prosthetic human tissue and wounds were developed for a realistic live training capability. A kit containing extremely realistic simulated wounds, or “moulage” was developed based on user requirements. Wound simulation, or “moulage,” is an integral part of scenariobased medical training, especially in live training. This kit allows for the quick and easy application of prosthetic entry, exit, and shrapnel wounds for live training exercises focused on enhancing realism.
Another technology developed under the Small Business Innovative Research (SBIR) program to support the ATO, introduced movement to enhance realism of the scenarios via animatronics technology. These two efforts are examples of technologies that have been commercialized and successfully transitioned to support the Warfighter. Research in severe trauma simulations continues with a focus on technologies to enhance realism and immersion to support training. Development of these technologies has greatly improved the realism of scenariobased training, effectively supporting the training of Army Combat Medics and allowing Soldiers to be immersed in relevant situations to conduct realistic, performance- based, hands-on training of hemorrhage control.
Teresita Sotomayor, Ph.D.
US ARL STTC
Donald Parsons, PA-C, MPAS
DCMT
teresita.sotomayor@us.army.mil
http://www.rdecom.army.mil/STTC
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.