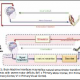
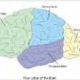
Setup of fNIRS (Functional Near Infrared Spectroscopy) and VR (Virtual Reality)
By Simone Cutini et al.
Virtual Reality (VR) is a useful tool in several fields and has reached a considerable value in medical, psychological, and neuropsychological treatments as it can be used for rehabilitating a broad variety of clinical populations, such as stroke patients (to recover gait or arm movements) or patients suffering from mental disorders (e.g. phobia or posttraumatic stress disorder). Indeed, several studies have shown that the same brain regions involved in these tasks in real life are also activated in the VR environment by mimicking the same task. In order to adjust and optimize the specific therapy required by each patient, it is mandatory to the improvements accomplished by the patient during his/her treatment. Qualitative data obtained through questionnaires and self-reported measures, as well as quantitative data registered during the interaction of the participant with the virtual environment can be easily collected.
However, they do not provide sufficient information: for instance, questionnaires do not inform how and where the neural recovery is taking place, and whether the improvement is temporary or permanent. A proper therapy should provide a permanent modification of the brain (thanks to its plasticity); thus, it is important to deeply understand the cerebral modification caused by rehabilitation techniques.
Brain imaging methods are the main tools that can provide such information. Despite their widespread use, functional magnetic resonance imaging (fMRI) and positron emission tomography (PET) present many disadvantages. Indeed, the bulky device, the loud noise, the horizontal and unnatural position of the participant, who is required to stay still for the former and the invasive use of radioactive tracers for the latter, are limiting factors for their use in a context of rehabilitation, even in a VR environment. The ideal brain imaging technique should be silent, should permit free movements of participants and should be non-invasive. Functional near-infrared spectroscopy (fNIRS) is a novel neuroimaging technique, which encompasses these features. It exploits the properties of light in the near-infrared range to detect cerebral activity. It is completely non invasive, less sensitive to motion artifacts and able to measure different cerebral parameters, which allow monitoring the modification of the brain regions during therapy.
Owing to recent advantages in the hardware development, wireless fNIRS devices have been recently proposed. The absence of cables makes these new devices even less sensitive to motion artifacts and allows the participant more freedom in his/her movements. The patient immersed in the virtual reality can easily move the body while performing the required tasks in the VR environment. This information is very important for physicians: fNIRS permits monitoring the brain during the therapy, while the patient is performing the exact task required during the rehabilitation session. Moreover, wireless fNIRS devices are so small that they can be carried like a bag. Children will obviously benefit from this feature, which, coupled with the virtual reality environment, can render the rehabilitation therapy less stressful and more comfortable. Encouragingly, the first studies combining fNIRS and VR provided positive results, making clear the capability of fNIRS to measure the cerebral signal while participants are moving in a virtual reality environment. In a recent study, we have shown that fNIRS is able to detect brain activity in the parieto-occipital region by participants wearing VR goggles during a line bisection task in an immersive VR environment; another investigation has shown that an interactive VR environment can properly elicit cortical oxygenation changes related to action observation. Another fNIRS study has investigated the prefrontal cortex response to virtual reality tasks that might be easily adopted in the field of functional neurorehabilitation. The participants were required to carry out an incremental and a control swing balance task in a semi-immersive VR environment, i.e. to try to maintain equilibrium on a virtual swing board susceptible to external perturbations (of different strengths in the former and of constant strength in the latter). Crucially, the authors found an increase in prefrontal cortex activity whilst carrying out the first task, thus highlighting the usefulness of fNIRS in these scenarios.
The combination of fNIRS and virtual reality is in its early days but it is clear how new hardware and software developments (e.g. improvements in signal processing techniques, in the hardware of the devices, in the virtual reality environment, etc.) will foster the use of fNIRS and VR for rehabilitation purposes. In conclusion, fNIRS is the neuroimaging technique that can provide the greatest flexibility, freedom of movements and comfort to the patients in a VR rehabilitation setting; at the same time, it can provide therapists valuable information for an optimal planning of the therapy.
Simone Cutini, Ph.D. Department of General Psychology Padua, Italy simone.cutini@unipd.it
Sabrina Brigadoi, Ph.D. Department of Developmental Psychology and Socialisation Padua, Italy
Pietro Scatturin Department of Developmental Psychology and Socialisation Padua, Italy
Luciano Gamberini, Ph.D. Human Inspired Technology Research Centre HIT University of Padua, Italy luciano.gamberini@gmail.com
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.