By Giuseppe Riva
For many of us, metabolic diseases are the outcome of an energy imbalance: more/less energy input than expenditure. However, our waistlines are growing in spite of the huge amount of treatments, diets and fatfree/ low-calorie products available to cope with them. As noted by many experts, “Fresh ideas are needed to push the field forward.” In this issue we have seen that a possible strategy for improving the actual treatment of metabolic diseases is the use of advanced information technologies. Specifically, different technologies – the Internet, Virtual Reality (VR), and mobile phones – have the potential to improve the assessment and treatment of these disturbances. Nevertheless, these devices are not perfect.
On one side, they typically try to change behaviors and cognitions at a more general level, rather than focusing on actual situations or the “real” context in which they happen. For example, even if VR is a very promising technology for the treatment of obesity and eating disorders, it is a distinct realm, separate from the emotions and behaviors experienced by the patient in the real world; the behavior of the patient in VR has no direct effect on real-life experiences, nor are the emotions and problems experienced by the patient in the real world directly addressed in the VR exposure.
On the other side, these devices are usually used in manualized approaches that allow for a limited amount of customization to be made according to the specific characteristics of a given patient. In real life, however, patients’ most immediate, pressing problem may change from week to week, and the technology is not usually able to effectively refocus on the new need or problem.
A possible path for solving these issues is the use of communication technologies to establish a link between the real world and the technological one: (a) the patient’s behavior in the physical world influences their experience in the technological world; and (b) the patient’s behavior using the technology influences their experience in the real world. Using this approach, usually defined as “Interreality,” it is possible to modify the patient’s relationship with his/her dysfunctional behavior and think through more contextualized, experiential processes.
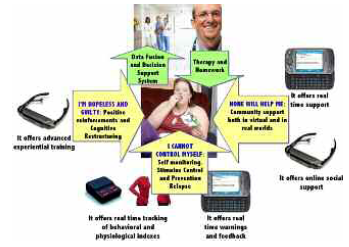
In summary, bridging multimedia experiences (fully controlled by the therapist, used to learn healthy behaviors and coping skills) with real experiences (the therapist can identify critical situations and assess coping skills in real life) – using advanced technologies (virtual worlds, advanced sensors and smartphones) may be a feasible way to address the complexity of these disturbances (see Figure 1).
Obviously, any new paradigm requires a large amount of effort and time in order to be assessed and properly used. Without a real clinical trial with patients, the Interreality paradigm will remain an interesting, but untested concept. However, direct and indirect costs of metabolic diseases are huge, and some new studies suggest that when managed and organized well, the use of Interreality technologies may lead to cost savings and improved outcome for both patients and health services.
Giuseppe Riva, Ph.D. Istituto Auxlogico Italiano Italy giuseppe.riva@unicatt.it auxo.psylab@auxologico.it
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.