➣ By Sam Sharar et al.
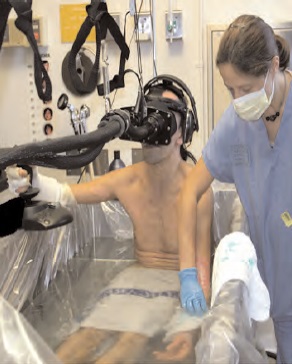
Figure 1: Burn-injured patient experiencing immersive virtual reality distraction while undergoing wound cleaning partially submerged in a hydrotank. (copyright Hunter Hoffman, University of Washington)
Since its inception in 1997, the Virtual Reality Analgesia Program at the University of Washington (Seattle, WA) has sought to explore and understand the mechanisms, efficacy, safety and cost-effectiveness of virtual reality (VR) applications to the vexing and unsolved problem of clinical pain. This commitment to exploring nonpharmacologic approaches to pain management is important because pharmacologic pain medications (e.g., opioids/narcotics) alone often fail to control the intense acute pain patients experience after injury, after surgery, or during medical procedures. Furthermore, such analgesic medications all produce dose-related side effects that limit the quantity of drug that can safely be administered – the result often being incomplete pain relief and other discomfort (e.g., nausea). Lastly, repeated episodes of excessive pain and the regular use of large doses of opioid analgesics can have serious long-term consequences, including increased risk of chronic pain and opioid dependence. Our program focuses on VR analgesia applications in clinical pain settings such as medical procedure-associated pain (e.g., wound care and rehabilitative physical therapy in patients with cutaneous burn injuries [Figure 1]), with a complementary laboratory research component whose two goals are to better understand the analgesic mechanisms of VR applications and to optimize their clinical use. Funding support for the program includes awards from the US National Institutes of Health, the Paul G. Allen Family Foundation, the International Anesthesia Research Foundation, the Scan-Design Inger/Jens Brun Foundation, and the Gustavus/ Louise Pfeiffer Research Foundation.
The most carefully studied analgesic approach to date is “VR distraction” – an approach based on the premise that the human pain experience requires conscious attention toward a painful stimulus (nociception). By immersing patients in an attention-grabbing, computer- generated, interactive virtual world that blocks the sights and sounds of the immediate medical care environment, their attention is pulled away from the concurrent painful stimulus of their injury or a therapeutic medical procedure, resulting in significantly reduced pain experience. Our group created an interactive virtual environment specifically for this purpose (SnowWorld® [Figure 2]), and published the first report of VR distraction analgesia in Pain in 2000. Subsequently we have reported clinical success with VR distraction analgesia in various clinical pain settings including patients with cutaneous burn injuries, dental pain, urologic surgery, and post-operative rehabilitation. Since 2007, our investigations have resulted in 38 peerreviewed publications in scientific journals, six textbook chapters and review articles, and one book, as well as collaborations for both clinical and research applications in civilian and military patient populations in ten centers in the US, Europe and the Middle East. Recently we have reported the first successful use of VR technology to facilitate hypnotic analgesia – inducing a hypnotic state and delivering hypnotic suggestions for reduced pain, improved function, and improved sleep – in patients with ongoing clinical pain following traumatic injuries.

Figure 2: Screenshot image of the user’s view of SnowWorld® during immersive virtual reality distraction. Virtual world designed/developed by Hunter Hoffman and David Patterson, with software created by Firsthand Technologies. (copyright Hunter Hoffman, University of Washington)
Complementary laboratory studies allow VR analgesia techniques to be studied in a controlled setting in healthy volunteers exposed to carefully regulated experimental pain. To better understand the neurobiology of pain and analgesia, we employ technically advanced outcome-assessment tools – for example, functional MRI imaging of pain-related brain activity and connectivity – and novel combinations of therapies (e.g., VR distraction combined with pharmacologic opioid receptor blockade) that are often not possible to study in the clinical setting. These investigations fill gaps in our knowledge of how new VR analgesic techniques work, and enable their exploration and refinement before they are introduced to actual clinical care. As a result of such laboratory studies, we have demonstrated that VR distraction produces similar reductions in both subjective pain reports and pain-related brain activity as intravenous opioid analgesics.
These studies have also helped identify the VR hardware and software components most essential to the user’s sense of presence in the virtual world, and hence the analgesic success of VR distraction.
Current efforts are exploring the relative roles of various central pain pathways and neurotransmitter systems, as well as the effect of user age (e.g., adolescent compared to older adults) on VR distraction analgesia.
Sam R.Sharar, M.D.
Harborview Medical Center
Department of Anesthesiology
Seattle, WA
USA
Hunter G. Hoffman Ph.D.
University of Washington
David R. Patterson Ph.D.
Harborview Medical Center
sharar@u.washington.edu
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.








