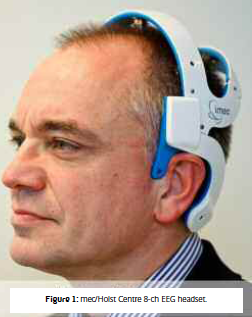
By Linsdsay Brown & Julien Penders
Healthcare systems are changing in response to new demographic factors including an aging society, increasing number of chronic diseases and a growing interest of individuals in managing their own health. Key trends include the evolution from disease centric to patient centric care, the delocalization of care from hospitals to home, and a focus on prevention rather than cure. This paradigm shift calls for new technologies to enable ubiquitous personal health. Body Area Networks play an important role in enabling this change by providing people with wireless wearable solutions ideal for personal health and lifestyle monitoring.
Using commercially available cardiac telemetry systems such as the Corventis NUVANT system, patients’ ECG can be continuously remotely monitored, with any adverse events being recorded and a physician notified for immediate care. These systems enable long-term patient monitoring out of the hospital environment, resulting in a higher quality of life for the patient.
Towards more assistive technologies, brain computer interfaces have taken a step further beyond simply monitoring and provide integrative functions for the patient. Today’s brain computer interfaces can interpret commands such as yes/no, and control machine response through changes in the level of concentration. Companies such as Emotiv and Neurosky exploit the same principle for improving the gaming experience.
In an effort to take EEG to the home environment, imec reported a wearable EEG headset (see Fig. 1) integrating dry electrodes. The EEG headset electronics have been optimized to cope with the specific challenges associated with dry electrodes, such as very high and varying input impedance. Optimized, ultralow- power electronics achieve over three days autonomy while wirelessly recording brain-waves.
Body area network technology is not limited to providing health monitoring and assistive functions. Research on cognition and information processing shows that physiological activity contains much more information than a physiological state or mental choice. Tapping into this information enables personal health devices to go beyond merely measuring activity and become health companions. For example, combining measurements of sleep with external factors such as caffeine intake, the My Zeo sleep coaching system allows users to monitor and improve their quality of sleep, in much the same way a person improves their fitness by exercising. The My Zeo system also provides interpretative functions in real time that enable the user to be woken up “smartly.” Using a different combination of sensors, a stress monitor may measure the physiological state related to stress and emotions. Employed appropriately, devices such as this can be used in many applications where stress and emotions influence actions and choices. For example, a stress monitor can be used to provide biofeedback on stress levels, enabling the user to maintain appropriate stress levels. Another example is a responsive photo frame that reflects the user’s level of arousal in real time using physiological measurements from wearable body area network sensors (see Fig. 2).
While providing excellent wearability and ease-of-use, often today’s devices are faced with making a trade-off between the overall wearability and ease-of-use of the system with the quality and accuracy of the signals and overall system. Current dry-electrode technology allows signals to be measured accurately at rest; however, challenges remain in their use during movement. Developing techniques for reducing motion artifact will enhance the robustness to motion artifact and thus overall accuracy during daily life activities. Similarly, often complicated algorithms are used in the interpretation of information, requiring high-computing power supplied only by a desk-top based device. Developing capabilities to process and integrate information at the sensor will enable local feedback to be provided directly by the wearable device. Further, today’s body area network devices are still limited to easy-to-measure signals such as ECG and skin conductance. Novel sensing technologies are needed to reliably measure more complex parameters such as chemical compounds and hormones, enabling greater insight into the physiological activity and condition. While these challenges seem trivial, they are made more complicated by the need to make these advancements in a way that further reduces power consumption beyond current levels. By reducing overall consumption, the autonomy of the wearable sensors is greatly increased, ensuring minimal maintenance by the user. And finally, while wearable today, future improvements in device integration and miniaturization combined with the added intelligence and reduction of power consumption, will enable the wearable sensors to become truly ubiquitous.
Imec’s Body Area Network research program addresses these key technology challenges with research focused on micro- power generation and storage, ultralow- power radios, ultra-low-power DSPs, ultra-low-power sensor technologies and advanced electronic integration. The ultimate target is a wearable device that can be used at home, in the office, in the car, anywhere, providing functions that enhance the users’ quality of life in health and/or lifestyle applications. That will become your health companion
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.