➣ By Mark L. Ryan et al.
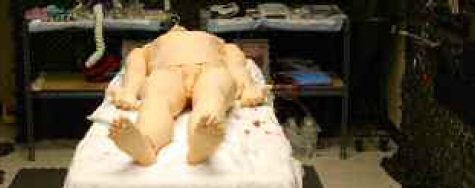
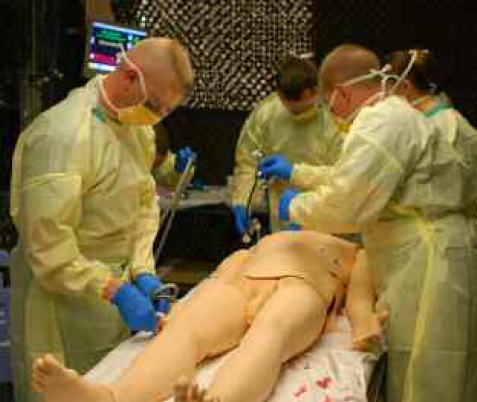
Figure 1: Simulation exercises are conducted in a recreation of a surgical tent similar to that used in the field.
Since September 2001, the Army Trauma Training Center (ATTC) at the University of Miami has provided instruction and training in the management of combat casualties for every Forward Surgical Team (FST) deployed to Iraq or Afghanistan. Each FST is composed of medics, nurses, and physicians with varying degrees of combat experience. It is therefore essential that teams receive intensive, focused training in clinical management, teamwork, and resource utilization in a controlled environment rather than on the battlefield. Participants are subjected to a two-week educational rotation composed of didactic instruction, cadaveric surgical exposure training, and a porcine-model mass-casualty exercise. An essential component of FST training involves simulation of acute injury using an advanced clinical simulator, the Sim- Man 3G.
The SimMan 3G (Laerdal Medical, Wappingers Falls, NY) is a patient simulation model with advanced clinical functionality combined with vital signs monitoring and an interactive software suite. It allows for testing and training in standard ACLS resuscitation protocols, as well as user-customized treatment scenarios. Mannequins are capable of manifesting clinical symptoms, such as pupillary dilation, eye secretions, blinking, breath and cardiac sounds, palpable pulses, convulsions, hemorrhage, and other signs of shock. Models also demonstrate physiological responses to treatment with medications as well as procedural interventions (chest decompression, intubation, ventilation, thoracentesis, defibrillation/ cardioversion, foley catheterization). The device has been deployed as an instructional tool in several U.S. Army Medical Simulation Training Centers around the world for the simulation of battlefield injuries.
At the ATTC, the SimMan 3G is utilized as an adjunct to the clinical instruction provided at Ryder Trauma Center, a level 1 trauma center located in Miami- Dade country with approximately 4,500 admissions per year and a high frequency of penetrating injury. Participants receive simulation training before starting the rotation and once more upon its completion. Prior to beginning the exercise, trainees are given the opportunity to survey the room and familiarize themselves with the equipment. They are then brought into an adjacent room, where they are informed of the patient’s mechanism of injury and provided a brief overview of their clinical status. The model is made to simulate a patient who has suffered either a blast injury or a gunshot wound. Participants are expected to rapidly address the patient’s injury while adhering to Advanced Trauma Life Support Protocols. Over the course of the exercise, progress is monitored by the instructor via a wireless tablet PC. The instructor is also able to input changes in clinical status to further challenge the team as necessary. The team then participates in an After Action Review (AAR) to evaluate their clinical performance. This simulation exercise serves as a valuable tool to assess team readiness prior to the initiation of their clinical duties, as well as for evaluating improvements in performance upon completion of their rotation.
Although the device has proven extremely useful for clinical simulation and team readiness, there are multiple scenarios for which the use of a simulator is not yet feasible. The limited portability of these devices has restricted their utility in our mass-casualty exercises, where rapid triage, treatment, and evacuation from the patient treatment areas are required to adequately simulate combat conditions. Also, there is currently no adequate simulation tool for the advanced operative management of battlefield injuries. A model capable of providing instruction in methods of hemorrhage control, organ exposure, and patient stabilization prior to evacuation would be extremely valuable in providing a consequence-free environment in which to hone these skills. Animal and cadaveric training are extremely expensive and labor-intensive. With current funding limitations and increased scrutiny of animal exercises, it is essential that novel, cost-effective simulation models are developed in order to alleviate our current dependence on these methods.
Mark L. Ryan, M.D.
Chad M. Thorson, M.D.
Christian A. Otero, M.D.
LT COL George D. Garcia, M.D.
University of Miami Miller School of Medicine, Ryder Trauma Center
U.S.A.
MRyan2@med.miami.edu
About Brenda Wiederhold
President of Virtual Reality Medical Institute (VRMI) in Brussels, Belgium.
Executive VP Virtual Reality Medical Center (VRMC), based in San Diego and Los Angeles, California.
CEO of Interactive Media Institute a 501c3 non-profit
Clinical Instructor in Department of Psychiatry at UCSD
Founder of CyberPsychology, CyberTherapy, & Social Networking Conference
Visiting Professor at Catholic University Milan.